
Can music therapy improve the sound environment for patients in hospitals? And how does it affect the patient experience when a healing sound environment is present? We’ve invited US-based Anne Taylor, CEO of Scandic Health and Registered Nurse. Scandic Health is offering music therapy, MusiCure – Music as Medicine, which is composed by the Danish composer Niels Eje in close collaboration with doctors and researchers.
The calming beat that’s hardwired into us
The basic primordial sound that we all have experienced is the sound of our mother’s heartbeat – relatively slow and peaceful. The link between the slow heart rhythm and the security of the womb is maintained throughout life. A calm heartbeat of around 60 beats per minute mimics the mother’s heart rate, which can generate a feeling of security, warmth, and comfort for many.
This calming beat has been present ever since mankind; the oldest evidence of music is a bone flute from around 45,000 years ago. The cave drawings in France show people dancing and it’s easy to imagine that the flute and maybe a drum was used to make healing music of some kind. (1)
It’s easy to imagine the humans in the caves used the flute during illness to calm the mind and reduce pain.
Music to relieve the stress experienced by patients
 Music therapy has a well-known and documented, relaxing effect. Research has shown chemical effects on the brain and body by the music used in healthcare. A study in Sweden found a 22% reduction in serum cortisol levels among post-op patients. The study found that 30 min of listening to specifically designed music could significantly reduce the stress level. (2)
Music therapy has a well-known and documented, relaxing effect. Research has shown chemical effects on the brain and body by the music used in healthcare. A study in Sweden found a 22% reduction in serum cortisol levels among post-op patients. The study found that 30 min of listening to specifically designed music could significantly reduce the stress level. (2)
Most patients are at the most vulnerable stage in their lives when facing illness and hospitalization. The fear, anxiety, and unknown situation diminish the patient’s ability to control their circumstances.
They lack the ability to control their circumstances.
Dr. Rana Awdish describes in her book In Shock the depersonalization that occurs when stricken with illness and hospitalized.
“Physicians often enter the lives of patients, on their absolute worst days. They meet without the benefit of social graces. They lack means to project their identity through dress or choice of hairstyle. They lack ability to control their circumstances. They might be in pain, scared and suffering. They might be worried about bills at home or who will feed the dog. They might be addicts. They might not have the skills to be kind while in pain. They might never in their lives have had kindness shown to them. They might have been abused or violated by someone they trusted. They might be many things.”
But one thing is true; they are doing their best. The patient, even the accusatory and fearful patient, is doing their best.” (3)
The patient’s loss of identity gets increased when deeply sedated and they lose the ability to communicate. They are dependent on family members to advocate and a compassionate and empathetic healthcare team.
Deep sedation takes the body and mind to a new level with:
- Absence of sensation
- Lack of memory
- In a dreamless stage
That’s how many patients are left to recover– like a ship on the open sea!
Our hearing – the open door
The sense of hearing is the only thing not muted in the deeply anaesthetised patient, the ear can be used to provide the patient with a ‘lifeline’ to reconnect back to life.
This ability has kept us alive; otherwise, we would have been eaten a long time ago by wild animals if we didn’t have ears that ‘stay open’ during sleep.
The brain’s music centre in the cerebral cortex is located close to the centre of emotions. There is ‘cross-talk’ between the emotions and the music centre; it makes it self-known when we get touched by certain music we listen to.
You can close your eyes but not your ears.
During sedation, the muscle in the inner ear does not have the capacity to change the stiffness as a response to noise.
With the patient’s ears constantly open, the noise in the unit can seem a lot louder to the sedated patient than to the family or staff at the bedside.
Time passed one slow second at a time, punctuated by constant beeps and the dull hum of machines. (3)
We can think of the ear functions as an open door. Through this door, we can stimulate the patient to dream, provide a lifeline of music and nature sounds back to life. Music becomes a co-therapy tool and a buffer to block out all the noise of a hospital.
Hospital noise and how the sound environment impacts the patients and staff
The noise comes from the machines, alarms, doors opening and closing, overhead announcements, staff talking, other patients, carts on wheels rolled down the hallway and the general noise of simply many people coming and going
Meanwhile, the body is searching for homoeostasis and healing. A very hard act to follow in a noisy environment!
Verbal and non- verbal communication is deeply impacted by the noise level in a hospital. A patient once told me “I notice when I have the TV on the medical staff talk so much louder when they enter the room; it’s like they want to overpower the sound from the TV, but when I have the calming music on they speak lower.”
Most patient rooms in the US are single private rooms and all with a TV. When you add the machines and the regular noise from the hallways, the noise level during the day can easily get up to a level the WHO compares to “a chainsaw going off next to your ear” kind of level; A measurement over 90 decibels compared to the WHO recommended maximum of 35-40 decibels.
A handy summary of research around noise in healthcare here.
Does the sound environment also impact the way we process facial expressions and our moods?
An international study from 2014 aimed to find out whether a relaxing or irritating sound environment affects implicit processing of facial expressions and how it affects the mood.
The main task of the study was a computer-administrated task on implicit emotion processing in which blocks of mixed angry, happy and neutral expressions from a validated set of facial pictures were presented.
Three different groups defined the sound environment:
- Music composed as medicine
- Noise
- Silence
Music as medicine:
This music has been specifically designed for therapeutic and relaxation purposes. It is a combination of neutral compositions mixed in with calming nature sounds, with a constant rhythm of 60 beats per minute to mimic the primal beat.
Noise:
The noise component was maintained from a MIRToolbox, which balanced the music as medicine amplitude content and also partially in the pitch content mixed in with a white noise signal.
Silence:
Without any sound in the background, the participants wore headphones.
The results – noise cause annoyance and anger
The researchers found that the music and the noise stimulus had comparable loudness but the music was less bright, less rough and clearer in its tone centres.
The impact on the mood was negative due to the noise and it mostly manifested in annoyance and anger. The participants reacted faster processing pictures of happy faces while listening to the music than angry faces while subjected to noise. (6)
The study concluded that the optimum healing sound environment has to be a place with less noise and where patients gravitate towards smiling faces and away from annoyance and anger. A healing environment sets a tone and signals a purpose for patients, family members and staff.
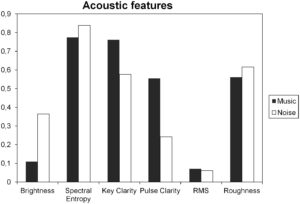
Figure 1. Acoustic features. Graph showing values of timbral (Brightness, RMS Energy and Roughness), rhythmic (Pulse Clarity) and tonal (Key Clarity) features of Music and Noise extracted with MIRToolbox. The Music resulted to have comparable loudness with the Noise stimulus but to be less bright, less rough and contain clearer tonal centres and pulse, as revealed by the mean parameters of Brightness, RMS, Key Clarity and Pulse Clarity, respectively. doi:10.1371/journal.pone.0103278.g001
Does music have a place in modern medicine?
Music in medicine is part of the connection back to life, back to memories and back to life after illness. Humans thrive on connection and that’s what specifically designed music provides.
Medicine cannot heal in a vacuum; It requires connection – Dr. Rana Awdish
The music and the natural sounds also mask the noise in the hospital by providing a connection to the primal beat, a calmer mind and a lifeline to recovery.
The evidence is there, the science has proven the positive effects of music and an improved sound environment will heavily impact the patient experience.
References
- Ancient music Ireland – Instruments through the arts ( ancientmusicireland.com)
- Nilson, U (2009) The effect of music intervention in stress response to cardiac surgery in a randomized trial. Heart & Lung May- June, 38
- Awdish, R First edition October 2017 In Shock 3,37,136
- Nilson, U, Rawal, N Unossan, M (1998) Music effects on the postoperative pain, 33
- Hole, J, Hirsh, M, Ball, E, Meads, C (2015) Music as an aid for postoperative recovery in adults. The Lancet, August
- Quarto, T, Blasi, G, Pallesen, K, Bertolino, A, Brattico, E (2014) Implicit processing of visual Emotions is affected by sound-induced affective states and individual affective traits. PLOS one, July.
About the writer:
- Name: Anne Taylor, CEO & Registered Nurse, Scandic Health
- Where do you live In Virginia right outside of Washington DC, USA
- Where do you go to find peace: The yoga room at my gym
- What’s your favourite sound: The Oboe played by Niels Eje
- How did you end up working with acoustics: A very personal recovery from mental illness introduced me to MusiCure – music as medicine and its evidence-based research on sound, healthcare and general mind calming.
- What is it like to work with room acoustics in your country: I thrive on promoting health and recovery, sharing my family’s story of healing has not only made me realise how big the need is for sound environment improvements to promote healing but it has also propelled me to continue to tell my story. As storytelling saves lives.
- What trends do you see in room acoustics: In the US the patient experience is in the spotlight as patients often ‘shop’ for which hospital to use, a star rating system is in place based on survey questions from past patients. One of the areas in the survey is noise as it pertains to healing. The better the patient experience, the better the star rating and ultimately the impacts show in the bottom line.


