
Room acoustics is an important factor to create sound, healing environments.
Having a proper indoor climate can raise productivity by more than 15%[1]
For more than a decade, ‘Evidence-Based Design (EBD) has been part of our DNA regarding building healthcare facilities. When it comes to the indoor climate we know that lighting, air quality, and acoustics are crucial parameters in healing architecture. Together with biophilic designs for the eye, the ear, and the mind.
Furthermore, we need to consider how our buildings can be more sustainable – the building material we use needs to have as little impact on the planet as possible, we need to secure profit – and last but not least, we need to build a sustainable and efficient environment for PEOPLE no matter where they are:
Office workers in a building with low-emitting products and good air quality scored 61% higher in the cognitive function test.[2]
Also in the education sector, we see the same trend and when it comes to acoustics we know that it affects teaching and learning massively and research also concludes that good acoustics lower heart rates[3].
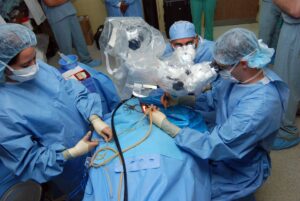
Patient issues
Let us look at the efficiency in the healthcare sector – what issues are we dealing with and what could the solutions be? Patients first.
In Denmark it is estimated that 10% of all patients get a bloodstream infection during a hospital stay – and there is a risk of 20% of dying because of that infection.[4] This is surely connected to a higher cost since the patient will have to stay longer in the hospital, getting more medicine, cure, and care. In Denmark it is tax-payers money – in other countries, it can be insurance money.
Infections and length of stay
Alone in American hospitals, the Centers for Disease Control (CDC) estimates that these healthcare-acquired infections (HCAI), also known as nosocomial infections, account for an estimated 1.7 million infections and 99,000 associated deaths each year and the annual economic impact was approximately US 6.5 billion.[5]
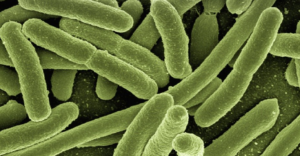 According to the WHO, HCAIs cause 16 million extra days of hospital stay in Europe and 37,000 attributable deaths and contribute to an additional 110,000, every year.[6] In a world where the risk of ‘super bugs’ is increasing, there is therefore a constant focus on the overuse of antibiotics and hygiene demands. Overuse of antibiotics is a topic in itself and can lead to a great healthcare crisis in general.
According to the WHO, HCAIs cause 16 million extra days of hospital stay in Europe and 37,000 attributable deaths and contribute to an additional 110,000, every year.[6] In a world where the risk of ‘super bugs’ is increasing, there is therefore a constant focus on the overuse of antibiotics and hygiene demands. Overuse of antibiotics is a topic in itself and can lead to a great healthcare crisis in general.
Indoor climate contributions
It is undoubtful that the indoor climate contributes either negatively or positively to these issues and it is undoubtful that the cost of EBD hospitals where room acoustics are prioritized is lower in the long run.
In a business case by Sadler et al.[7] less noise was considered to contribute to fewer adverse drug effects and reduced nursing turnover at the same time as noise reduction by installing acoustic ceilings and wall panels contributed to less sleep deprivation, quicker recovery, and decreased stress (high-performance acoustic ceilings were used in all patient care areas). Finally, in this case, the premium for EBD was estimated at 7.2% of the total building cost AND the payback time for EBD at this hospital was estimated at only 3 years!

Room acoustics are crucial
When it comes to sound and acoustics we know that patients, no matter if they have just gone through serious heart surgery or suffering from pneumonia need to recover quickly to avoid infections – and successful recovery is based on sleep. Sleep, unfortunately, is a luxury in healthcare facilities of today that have become small cities that work around the clock. It is estimated that the average restorative period for a patient in the ICU is as short as 6.2 minutes![8]
Sound levels
Since the 60ies, actual sound pressure levels have increased in level – both during daytime and nighttime – and it is not unusual to have

sound pressure levels sufficiently high to interfere with sleep, affect speech intelligibility, and create a level of background noise that will annoy and affect most people.[9]
A noisy healthcare facility where the room acoustics don’t support the activities will never be efficient – and the result will be more patient infections[10], more medication[11], and healthcare staff that cannot perform. Let us look at how the staff is affected by sound and acoustics.
Staff issues
…sometimes I’m not sure if they don’t hear what I’m saying or if they don’t understand what I’m saying![12]
Neurologist in Denmark working with people with dementia.
Noise levels can make it impossible for staff members to diagnose correctly at the same time as the patients don’t always hear what the caregiver said. Because of demographic changes we see older and older people in our healthcare facilities and because of age-related hearing loss and sometimes cognitive deficits it is harder for the staff members to receive the correct information from the patient. This can lead to mistakes and the patient cannot always hear because of poor acoustics and the answers will not be fulfilling.
Mistakes increase with bad acoustics
In general, our bodies and brains have developed for the outdoors. If we compare the time we have lived outdoors as cavemen to the time we have been living inside – we see a huge difference in time. Our hearing has not changed since we lived outside, and in this environment we needed our hearing to survive – if we didn’t react we would die. We needed both to react to the information in the sound (was it an animal or just the wind?) as well as the loudness to know whether to react, fight, fight, or flee.
Healthcare staff is often working in conditions where fast decisions and precision work are key factors to an efficient treatment. Unfortunately, the sound environment can play a negative role if the acoustics are not supporting the activities and the ‘caveman’ of the caregiver will be challenged.
Mistakes in the operation room

In a hospital in Denmark, staff members working in three similar (m2, geometry, equipment, etc.) operation rooms stated that the room acoustic treatment of the facilities affected them[13]. The three rooms were designed with different acoustic treatments – going from minimum treatment (acoustic ceiling – absorption class C) to medium treatment (acoustic ceiling – absorption class A) to maximum treatment (acoustic ceiling and wall panels – absorption class A).
Results from a questionnaire revealed that the staff members were more likely to make mistakes in the operation room with less acoustic treatment and the communication events in the same room were also troublesome:
I don’t know where the sound is coming from – I cannot orient.[14]
Operation Nurse about the less-treated room.
Mistake leads to respiratory arrest
In an advisory report based on healthcare staff reporting to the PAPSRS (Pennsylvania Patient Safety Reporting System (USA)) many examples of real-life medical errors due to mishearing were found[15].
Knowing that the only real record of a verbal order is in the memories of those involved it was not surprising to find that background noise and interruptions because of sound peaks could lead to mistakes. Some of the reported mistakes were as follows:
- An emergency room physician verbally ordered ‘morphine 2 mg IV’ but the nurse heard ‘morphine 10 mg IV. The patient received a 10 mg injection and developed respiratory arrest.
- A physician called in an order for ‘15 mg’ of hydralazine to be given IV every 2 hours. The nurse, thinking that he had said ‘50 mg’ administered an overdose to the patient who developed tachycardia and had a significant drop in blood pressure.
- A phone order mistaken for Toradol 50 mg was administered before the pharmacy review when the intended dose was 15 mg.
Healthcare efficiency, sound, and acoustics

The healthcare sector is complex no matter where you go, we will see more and more people in the facilities and more and more tasks to solve, and room acoustics play just one part in the big play. However, the investment in room acoustics seems to make sense. If you compare the money you spend on this with the benefits you gain, it is a sustainable investment in efficiency – even without data and research saying that you the payback time is only 3 years![16]
Patients sleep better, heal better, get fewer infections and get well faster if they are in calm sound environments and staff performs better with fewer mistakes in working environments where the communication is clear and the background noise is low.
____________________________________________
[1] Harvard Business School (2016)
[2] David P. Wyon and Pawel Wargocki, “Effects of the indoor environment on performance”, ASHRAE Journal (2013)
[3] Tiesler and Oberdöster, Acoustic ergonomics of school (2006)
[4] Numbers from ’Sundhedsdatastyrelsen’: https://sundhedsdatastyrelsen.dk/da/tal-og-analyser
[5] Numbers from PatientCareLink (PCL) which is a patient safety and healthcare quality initiative for patients, families, and healthcare providers.
[6] WHO: The Burden of Health Care-Associated Infections Worldwide
[7] Sadler et al., “Fable Hospital 2.0: The Business Case for Building Better Health Care Facilities,” Hastings Center Report (2011)
[8] Lange et al: The sound of the intensive care unit – 3 weeks of continuous sound recording (2015)
[9] Busch-Vishniac et al., “Noise Levels in John Hopkins Hospital”, Journal of the Acoustical Society of America (2005)
[10] Salonen, Heid et al., “Design approaches for promoting beneficial indoor environments in healthcare facilities : a review”. Intelligent Buildings International (2013)
[11] Minckley, “A study of noise and its relationship to patient discomfort in the recovery room”, Nursing Research, (1968)
Hagerman et al., “Influence of intensive coronary care acoustics on the quality of care and physiological state of patients”, International Journal of Cardiology, (2005)
[12] Qupersimat, R. Intervention study of room acoustics at the dementia clinic in Århus university hospital, 2019
[13] Beldam, “Impact of acoustics on staff performance in operation rooms”, Internoise, Madrid, 2019
[14] Ibid
[15] Pennsylvania patient safety authority, “Improving the safety of telephone or verbal orders”, PA-PSRS Patient Safety Advisory, (2006)
[16] See 7

